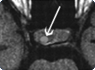
Rathke’s Cyst: Endoscopic Skull Base Surgery through the Nostril
One of the most extraordinary advances pioneered at the Skull Base Institute is the minimally invasive, fully endoscopic approach to the skull base. Sellar and suprasellar lesions such as Rathke’s cyst and other skull base disorders are routinely removed through this approach. This innovative procedure utilizes a tiny endoscope – 2.7 mm wide and 20 cm long – with angled tips that is inserted through the nostril and into the skull base. This approach offers numerous advantages in terms of the surgery and recovery period.
Since the point of entry is through a nostril, no incision is required. Consequently, there is no scarring, no nasal packing, and the brain is undisturbed. The time required for the actual surgical procedure, the length of hospital stay and overall recovery time are dramatically reduced. Patients return home within 24-48 hours of surgery and enjoy a rapid overall recovery, and return to work and normal activities. Today, our research and development is focused on yet further innovating the field of Minimally Invasive Brain and Skull Base surgery. High definition intraoperative digital imaging, 3D endoscopy, custom designed microinstruments, heads-up displays and even nanotechnology are all being tapped in order to provide our patients with the most cutting edge and yet least invasive approaches to rid them of their tumors.
Overview
Rathke’s cyst, or Rathke cleft cyst (RCC), is a benign epithelium-lined cyst, that arises primarily within the sella turcica and is thought to originate from remnants of the Rathke’s pouch (Rathke’s pouch is the primordium of the anterior and intermediate lobes of the pituitary gland).
The cyst is lined with a single layer of epithelium and has a thin and transparent capsule. The fluid within the cyst is usually yellowish in color but can also be clear, grayish or bluish, it may be thick or gelatinous, but it also can be watery, serous, or similar to motor oil in consistency. The cyst is found incidentally in 13-23% of autopsies, and may be completely asymptomatic. Symptomatic RCCs have been reported to occur in patients of all ages and to be more common in females than males. The patient’s age at presentation may range from 2-72 years but the highest frequency is in those aged 50-60 years. No racial predilection is recognized.
Causes
Rathke’s cyst is congenital in origin, although its pathogenesis is by no mean clear; it is generally believed that the cells of origin are the remnants of Rathke’s pouch. The adenohypophysis (the anterior glandular part of the pituitary gland) is also driven embryologically from the anterior wall of Rathke’s pouch and so RCCs have a similar lineage to that of a pituitary adenoma, and rarely both lesions may occur in concurrency.
Symptoms
These benign cysts are often discovered incidentally and may not produce any symptoms, but RCCs can enlarge and cause symptoms secondary to compression of the pituitary gland, pituitary stalk, optic chiasm, or hypothalamus. The common clinical presentation includes headache, visual impairment, and endocrine disorders.
The most common endocrine disturbance is pituitary hypofunction, but other forms of endocrinopathies may also occur. They may compress the pituitary stalk causing diabetes insipidus, or hyperprolactinemia. Diabetes inspidus (DI) is a disorder that Causes increased urination (polyuria) and increased thirst. Hyperproclactinemia, in women Causes amenorrhea and/or galactorrhea and in men impotence and low libido. Visual symptoms include reduced visual acuity, optic atrophy, visual field defects, or hemianopias. Less commonly, Rathke’s cyst may present with seizures or occur in association with a pituitary adenoma.
Diagnosis
The diagnosis is generally entertained either on the basis of visual problems arising from the compression of the optic nerve(s) by the cyst, or on the basis of endocrinal manifestations. The diagnostic evaluation for Rathke’s cyst includes precontrast and postcontrast MRI/MRA and CT scans, endocrinologic and neuro-ophthalmologic evaluation.
MRI with thin-sections through the sella turcica is the modality of choice for detection and evaluation of RCCs. RCCs are usually located in the midline within the sella turcica and may have a suprasellar extension, the pituitary stalk and gland are usually displaced posterior. The cyst usually ranges in size from 2-4 cm and has the appearance of a well-circumscribed, cystic mass with a thin wall that may enhance. MRI has superior multiplanar capabilities and contrast resolution compared to that of CT, thus it can display reliable information concerning the relationship of the cyst to the optic nerves, pituitary gland and hypothalamus as well as its lateral extension and relation to the internal carotid arteries and cavernous sinuses.
CT scan is useful in evaluating any associated bony remodeling induced by the cyst and in assessing for the presence of calcification. The advantage of CT is its ability to depict small amounts of calcium; this advantage can be important because the presence of calcification tends to indicate an alternative diagnosis such as craniopharyngioma, although small calcifications are sometimes observed in some cases of RCCs.
As a result of the variability in its appearance imaging techniques alone cannot support a definite diagnosis of RCC. Simple cysts may be indistinguishable from arachnoid cysts or epidermoids. More complex cysts may be indistinguishable from a craniopharyngioma or a pituitary adenoma. For this reason, definite diagnosis must be supported by clinical and pathologic findings.
Neuroopthalmological and endocrinological evaluation are important as visual affection and endocrinal disorders are the major clinical presentation of symptomatic Rathke’s cysts.
Treatment
Because these cysts are often asymptomatic only patients with clear neurological and endocrinological indications require treatment. The most common approach in the treatment of RCCs is trans-sphenoidal surgery, in which the cyst is partially excised and drained, or less commonly a formal craniotomy is performed, usually via a right frontal bone flap to access the cyst. In both case simple cyst aspiration is not recommended as it may readily recur. Radiation therapy has no role in treatment of these benign lesions.
Prognosis
Surgical good prognosis and the recurrence rate has been reported to be less than 5%. The postoperative outcome of most patients is resolution or improvement of their symptoms. Early detection and treatment, , is associated with a better clinical outcome as long standing endocrinopathies or visual impairment are less likely to resolve completely and may become permanent.
If you or someone you love has questions about Rathke’s Cyst, please Contact Us and we will be happy to help you.
