Quick Launch Topics
Three Minimally Invasive Endoscopic Approaches to Craniopharyngiomas
Traditionally, open surgery has been the main treatment for craniopharyngiomas. However, at the Skull Base Institute, three different minimally invasive endoscopic procedures allow us to tailor the procedure offered depending on the size and location of the tumor. For completely intrasellar craniopharyngiomas with no suprasellar extensions and no significant attachments to the optic chiasm, endoscopic transnasal approaches similar to those offered for pituitary tumors are also offered for these craniopharyngiomas. Craniopharyngiomas located in the suprasellar areas with adhesions to the optic chiasm are approached through a minimally invasive endoscopic approach by placing an incision within the skin crease in the bridge of the nose and by performing a one centimeter keyhole midline frontal craniotomy. Under direct vision the tumor along with its adhesions to the chiasm is dissected and completely resected. This minimally invasive endoscopic frontal craniotomy approach is ideal for most craniopharyngiomas since they invariably extend to the suprasellar area and also invariably have adhesions to the chiasm. Patients are discharged within twenty-four to forty-eight hours.
Occasionally, craniopharyngiomas extend laterally beyond the midline. Craniopharyngiomas that extend laterally are approached through the most recent technical innovation at the Skull Base Institute, this fully endoscopic approach involves placing an incision within the hair of the eyebrow, performing a 1-1.5cm keyhole supraorbital opening and advancing the endoscope along the floor of the anterior cranial fossa underneath the frontal lobe. This approach allows a panoramic visualization of the ipsilateral anterior fossa and a partial visualization of the contralateral anterior fossa.
Although most craniopharyngiomas are completely resected through one of these minimally invasive approaches, occasionally giant lesions may require a combination of the endoscopic transnasal approach with either the endoscopic frontal approach or the endoscopic supraorbital approach. This can either be done simultaneously or can be staged as two separate procedures. This allows a complete and total resection of virtually most craniopharyngiomas from small completely intrasellar lesions all the way to giant craniopharyngiomas extending to the suprasellar area and also spilling laterally into the base of the anterior or middle cranial fossae.
Overview
Craniopharyngiomas are histologically benign (non-cancerous), extraaxial (extrinsic to the brain), slow-growing tumors that occur exclusively in the region of the sella turcia (a bony depression located at the base of the skull where the pituitary gland resides) and are thought to be derived from squamous cell nests of the hypohyseal stalk, which connects the pituitary gland to the brain (hypothalamus).
Craniopharyngiomas may be intrasellar or suprasellar and may cause various degrees of hypopituitarism by compression of the adenohypohysis (the anterior part of the pituitary gland), pituitary stalk or the hypothalamus.
Craniopharyngiomas are uniformly benign and they produce no hormones, they can be solid, cystic (full of fluid) or full of debris, they may show various degrees of calcification or bone formation. Due to their slow-growing characteristics, these tumors can take years to manifest themselves before a diagnosis is made.
Craniopharyngiomas account for approximately 2 – 3 % of all intracranial neoplasms and are most common in childhood and adolescence; their peak age of discovery is between 5 -10 years and they represent 5 – 13% of all brain tumors occurring in children. There is no sexual predisposition and both males and females are affected equally. Despite its histologic appearance, craniopharyngiomas may rarely behave like malignant tumors and can metastasize.
Causes
Craniopharyngiomas are congenital in origin. The craniopharyngeal duct (connecting the brain to the pharynx), is the embryonal structure along which the eventual adenohypophysis and infundibulum migrate. This explains the name of the tumor (cranio=skull, pharynx=throat, oma=tumor). The trigger that initiates tumor growth is not known.
Symptoms
A craniopharyngioma is a benign tumor that develops near the pituitary gland. Craniopharyngiomas cause symptoms in three different ways: 1) by increasing the pressure on the brain (intracranial pressure) 2) by disrupting the function of the pituitary gland, and 3) by damaging the optic pathways. Increased pressure on the brain Causes headache, nausea, vomiting and difficulty with balance.
The clinical presentation of craniopharyngioma patients consists of a broad spectrum of symptoms that range from completely asymptomatic (incidentally discovered) to endocrine, visual, or psychological disorders. Many patients remain asymptomatic for long periods of time, while others have a progressively deteriorating clinical course.
The symptoms associated with a craniopharyngioma are related to its location and size. They include symptoms related to an increase in the intracranial pressure (ICP) due to blockage of cerebrospinal fluid (CSF) pathways causing headache, nausea, vomiting and difficulty with balance; and symptoms related to direct pressure they exert on the surrounding neurovascular structures such as decreased vision, particularly peripheral vision due to direct pressure on the optic nerves. They may also cause hormonal manifestations due to pressure on the hypothalamus and pituitary gland causing obesity, excessive thirst and urination (diabetes insipidus), stunted growth and delayed developmental milestones.
Diagnosis
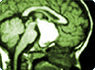
A thorough medical history and neurological examination are the first steps in the diagnosis. Complete radiological investigations to select the proper treatment protocol and identify tumors that may require staged surgical operations, and to denote the size and extent of the craniopharyngioma, must then follow. The imaging tests include magnetic resonance imaging (MRI) and computed tomography (CT) scanning both performed with and without intravenous contrast.
Due to the frequently associated visual and endocrine dysfunction with craniopharyngiomas, an ophthalmological and endocrinological baseline evaluation is frequently performed.
Treatment
Traditionally, surgery has been the main treatment for craniopharyngiomas. However, radiation therapy (conventional or gamma knife (GK)) and intra-tumoral chemotherapy may be applicable for some patients. Sometimes these treatments may be combined especially in cases of residual tumor following surgery. If possible, radiation and chemotherapy is withheld in younger children to prevent their delayed side effects.
Prognosis
In general the prognosis is good, but it depends on several factors, including the ability of the tumor to be completely removed, and the neurological deficits and hormonal imbalances caused by the tumor at time of treatment.
As craniopharyngiomas are primarily tumors of childhood and the usual course is progressive, early treatment avoids the occurrence of undesired complications.
If you or someone you love has questions about Craniopharyngioma, please Contact Us and we will be happy to help you.
